 It is my custom and practice to call the patient the night before surgery, to brief them on the answers to the “pop quiz”, which out admitting RN asks.
It is my custom and practice to call the patient the night before surgery, to brief them on the answers to the “pop quiz”, which out admitting RN asks.
Patients are gratified to have a preview so that they can ease into the surgical day, as effortlessly as possible. I aim to decrease their anxiety and accordingly, make the day’s work flow easier. Not an easy task, as even the most relaxed individual must conquer pre-op anxiety before climbing onto the OR table. Lines, equipment and IVs are placed and before the Anesthetist’s infusion of Morpheus induces sleep, there is a short corridor of disinhibition, in which some noteworthy murmurs are overheard. Some young mothers are assuaged with grief, “Please let me wake up, I have children”. Initially this ambivalence alarmed me, however armed with the knowledge that all aspects of pre-op planning, patient selection and staff support are optimized, I confidently respond, “yes, you will wake up, at the right time, at operation’s end. You’ll return home, at day’s end, and so will I.”
My practice focus has gravitated to cosmetic or elective surgery. To those who are curious, my definition runs something like this: “It’s when a basically healthy person is made temporarily worse, from physical and psychological aspects, because both patient and surgeon believe they can produce a “better outcome.” Accordingly, the time between waking and twilight sleep is when many of the patient’s deepest thoughts, fears, impressions percolate up to the surface. Sometimes an indiscretion may be uttered, “Please let my ‘friend’ know how I did, as well as my husband.” We are bound to the highest standards of discretion and subliminal requests are honored. Not infrequently declarations of respect and love are murmured and remind all members of the surgical team how deeply our patients trust our stewardship. Never knowing how much intra-op recall persists, I usually respond, “visualize a place of tranquility, as you sleep and your waking will be serene.”
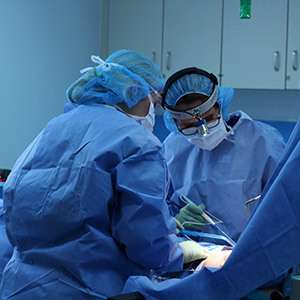
Analogous to a flight, where take-off and landing require substantial teamwork, an operative procedure demands supreme teamwork. The rationale from the Circulating RN’s announcement of the “flight plan” before the patient is asleep is to ensure the patient identity is confirmed, allergies and operative plan recognized; in short to avoid medical errors. All support is given to the Anesthetist during induction (going to sleep) and reversal (waking up). During the “flight”, the topic of conversation invariably centers on the phases of the procedure, requesting instruments, positioning implants, dressings, projecting “time estimate” for its conclusion. My concentration is targeted and the priority of safe passage and accomplishing the mission always respected. An OR is not silent like a place of worship, however the focus always reverts to the patient, whose vital functions emanate from the melodies issuing from blood pressure, electrocardiogram and Oxygen saturation monitors; the cacophony of living physiology is literally “white noise” for me. Occasionally a patient may make purposeful movements, suggesting that their level of comfort is not being met. The Anesthetist is always present, listening and vigilantly administering supplemental doses of medicines as the patient’s needs require. Upon waking, some wonder whether they snored or divulged anything and our response is emphatically, “nothing unusual.”